Do You Need A 3D-Printing Ovary
Date:25-07-2017 | 【Print】 【close】
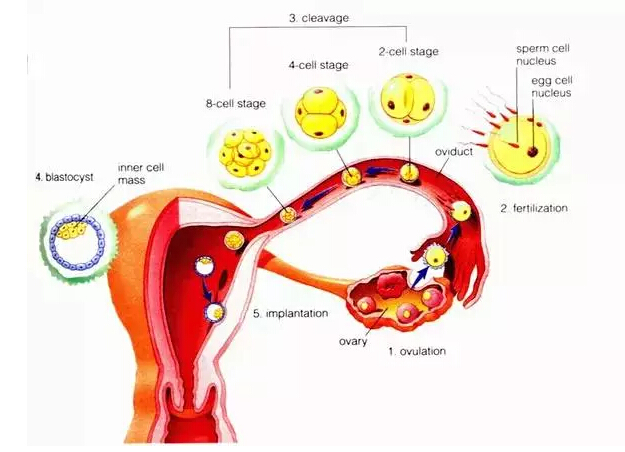
Where do I come from?
Under normal circumstances, mature women have different sizes of follicles in pair of their ovaries, and every month an egg, when it is mature, would be released from the follicle into the fallopian tube.
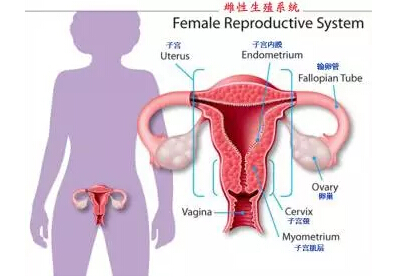
Female reproductive system section pic.
Egg travels down and reaches the ampulla of fallopian tube, quietly waiting for a sperm. There is an extremely denser layer called zona pellucida surrounding the egg. And a sperm needs to use its own "head" (professional term called the acrosome) to fuss with the zona pellucida so it could penetrate the egg in order to fertilize it.

A group of particularly strong sperm running toward ovary
When a group of particularly strong sperm arrive in the ampulla of fallopian tube, all sperm want to bind to the zona pellucida, but only one sperm cell can penetrate the zona pellucida. After that, zona pellucida will be hardened, preventing additional sperm from binding to or penetrating it.
A fertilized egg will be formed because of the joining of an egg and a sperm. It then divides and becomes a blastocyst. And the already fertilized egg will adhere to the wall of the uterus, which is known as implantation. Medically, implantation problems often occur and many details during this process are yet to find out. Dr. ZHANG Jian is hoping to help solve some of the problems by using 3D bioprinting technology.
At the very beginning, the fertilized egg is just a single cell, and it then slowly divides into two, four, eight, sixteen cells. Initially, the fertilized egg undergoes a series of cleavage divisions, as the number of cells increases, trophoblast cells are present, which will attach to the uterine lining and develop into a large part of the placenta. Another clump of cells would become inner cell mass (ICM) and eventually give rise to the fetus.
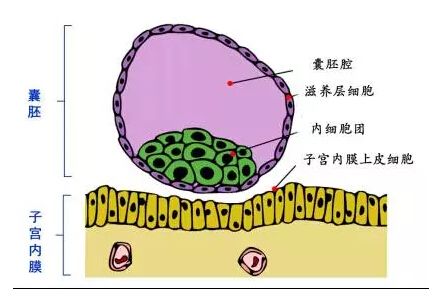
People often say that the first 3 months of pregnancy is particularly important, because the embryo, mainly trophoblast cells, is busy building “relationship” with endometrium, trying to be completely embedded in the to endometrium to form placenta. If it fails to do so, miscarriages or preterm labor are likely to occur.
Because the uterus is like a "black box", it’s hard to study the implantation process and explain the complex and sophisticated interaction between embryo and endometrium by visualizing the uterus with a noninvasive approach.
Research 1: 3D bio-printing of functional endometrium
Dr. Zhang and her team are currently using 3D bio-printing technology to print out a functional endometrium, aiming to study the process of the interaction between embryo and endometrial.
If this technique succeeds, it will be another visualization model for this research after years‘ work with 2D, 3D and scaffold cultivation models to help us further understand the key factors in the interaction between embryo and endometrium and also acts like a research tool to identify and discover the causes and intervention strategies for clinical preterm labor, recurrent spontaneous miscarriage(RSM), uterine adhesions, thin endometrial lining and other diseases.

3D printing endometrial model map (Pictures come from the Prof. REN Peigen)
Research 2: 3D bio-printing of functional ovary
The uterine lining will begin to shed about 10 days from ovulation if fertilization does not take place, and the period comes. At the same time, the estrogen and progesterone secreted by ovaries will stimulate the growth of follicles.
In the menstrual cycle, some women may have polycystic ovaries (prevalence rate of 15% -20%), due to the accumulation of immature follicles on their ovaries, while a lack of of follicles (called failure of activation of primordial follicles), can happen to women with premature ovarian failure (POF) / ovarian dysfunction, ovarian cancer, or postmenopausal women.
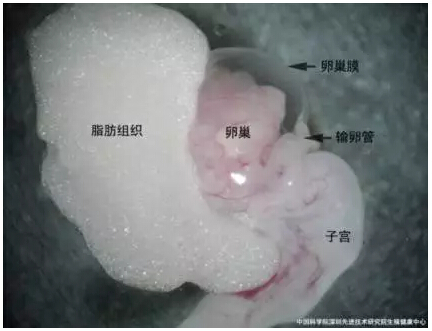
The related tissues of the reproductive system in mice (Pictures come from the Dr. ZHAO Huashan from SIAT)
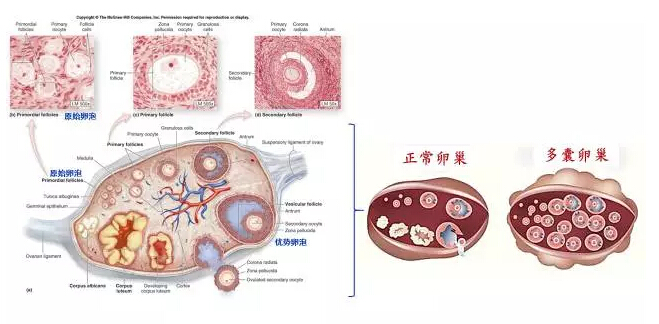
Patterns of normal ovaries and polycystic ovaries
Tips: A woman can ovulate about 300-400 eggs in her lifetime, and she is born with all the eggs. Ovaries contain primordial follicles, only a small number of which will be selected into the growing follicle pool and
has the opportunity to become the dominant follicle to release eggs.
This is also a difference between men and women. The process of sperm production is continuous, and involves several steps that lead to the differentiation of cells into functioning sperm cells. The epididymis store sperm that undergo maturation processes, and even the vas deferens carries a small number of mature sperm. It takes 3 months for sperm to mature before they are ready for ejaculation, therefore the sperm production is a continuous and uninterrupted process. There are always little warriors in every battle. If you lack of sleep in the last three months, the sperm quality might be lowered, but don’t worry, new ones will be produced in the next three months.
Dr. ZHANG Jian and the team are currently working on using 3D bio-printing technology to print out a “scaffold", which is made of biomaterials and to which the neurotrophic factors are immobilized. This scaffold can support follicles activation and development. They plan to incorporate a patient’s cortical fragments containing dormant follicles into this scaffold, and then transplant this "artificial ovary" to the patient, so that patient can restore fertility. For patient who is preparing for pregnancy, mature egg or eggs will be removed from the patient’s body, fertilized with sperm in vitro fertilization, and then transplanted back to the uterus. It is known as Assisted Reproductive Technology, or Test-tube baby procedure.

The difficulties of this technology lie in:
1. Materials science
The hardness and flexibility of the materials should be controlled, neither too hard nor too soft material is suitable for printing. In addition, biocompatible and harmless material is required. After the transplantation, the scaffold should be able to degrade, and provide sufficient space for follicles to fully grow. Materials like collagen matrix are often used to support the structure and maintaining flexibility and materials, such as inorganic salts, organic salts, sodium alginate, and nutrient fluid can be used for water and salt supply ; Besides, cytokine, which is expensive, is often utilized. For different purposes and requirements, the composition and proportion of the materials are different.
2. Biology
The use of 3D printing in the biological field is far less widely used compare to that in the industry. Because it involves the complexity of the organs and how printing materials and organs match. Especially we have to ensure that the printed organs are "live", professional speaking, we want to print out functional organs. The outstanding quality in 3D printing depends on the temperature, humidity and pressure control. Besides, how to supply the printing tissues with nutrition and blood should be fully considered.
3. Computer science
The team needs to design and create a 3D scene that mimics functional endometrium for follicles to grow, premix the materials, and use pretty printing to achieve dimensional accuracy.
4. Printer
The project team is currently using the 3D bioprinter (Bioscaffolder3.1, GeSiM, Germany) from Dr. RUAN Changshun research group, which can either print out the structures according to a given image or modify some parameters to create a more complicated spatial configuration. In the future, there will be upgraded bioprinters with more precise and impressive features for artificial ovaries, endometrium and other artificial tissues and organs to be more functional.
Contact:
Prof. ZHANG Jian
Prof. YANG Yali
Editor: ZHANG Xiaomin